Skin conditions often happen to people and usually, they don’t bother us much. Some may cause itchiness or irritation but most of the time, they are just there – a small cosmetic problem that we can live with.
But then there are skin conditions that are more than just cosmetic problems. They can be painful, itchy, and downright embarrassing. One such condition is keratosis pilaris (KP).
Table of Contents
What is keratosis pilaris?
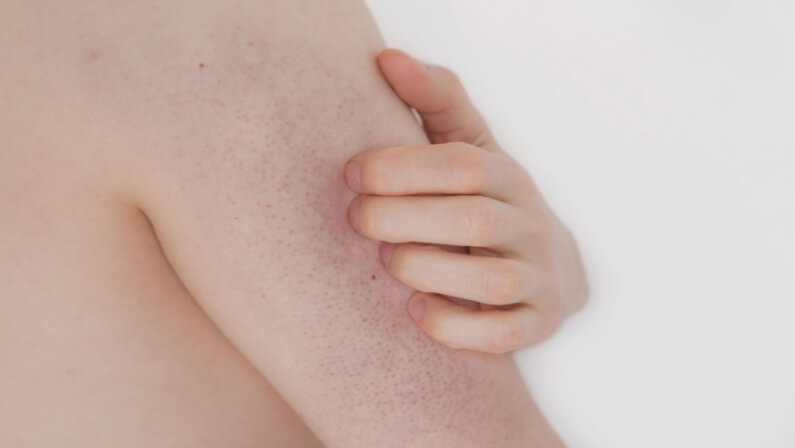
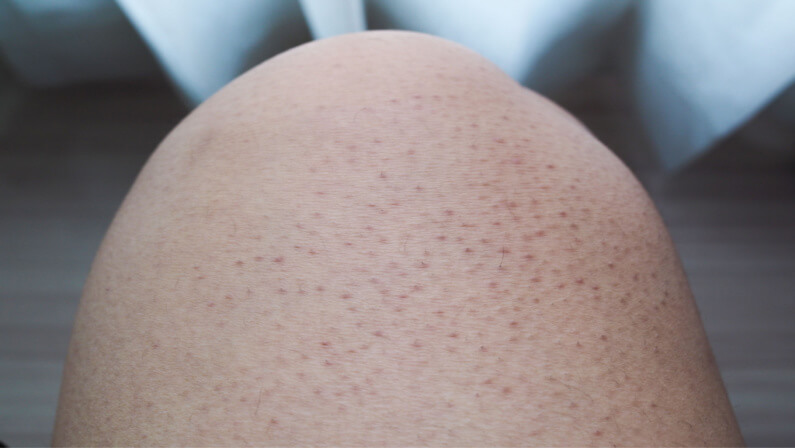
Keratosis pilaris is a skin condition that causes small bumps to form on the skin. These bumps are often red, white, or yellow in color and they can be very itchy. KP is a very common skin condition – it affects about 40% of the population – but it is often misunderstood.
Moreover, KP is often confused with other skin conditions, such as acne, eczema, and psoriasis. This can make it difficult to diagnose and treat.
In this article, we will discuss everything you need to know about keratosis pilaris. We will talk about what it is, what causes it, and how you can treat it.
Who can develop keratosis pilaris?
Keratosis pilaris can affect anyone, but it is most common in children and adolescents. KP often goes away on its own as a person gets older, but some people never outgrow it.
Is keratosis pilaris contagious?
No, keratosis pilaris is not contagious. You can’t catch it from another person and you can’t pass it on to someone else.
However, KP is often genetic. This means that if you have KP, there is a good chance that someone in your family also has it.
Causes of keratosis pilaris
The exact cause of KP is unknown, but it is thought to be related to a buildup of keratin on the skin.
Here are some common causes of KP:
- Dry skin. People with dry skin are more likely to develop KP. This is because dry skin can lead to a buildup of keratin on the skin.
- Genetics. As we mentioned, KP often runs in families. If someone in your family has KP, you are more likely to have it as well.
- Hormonal changes. Hormonal changes, such as those that occur during puberty or pregnancy, can trigger KP.
How keratosis pilaris is diagnosed?
Here is how keratosis pilaris diagnosed:
Doctor asks about your medical history.
Doctors are likely to ask about your medical history and your family’s medical history. This is because KP often runs in families.
The doctor does a physical examination.
A physical examination is usually all that is needed to diagnose KP. Your doctor will look for the characteristic bumps on your skin.
The doctor may do a skin biopsy.
In some cases, a skin biopsy may be necessary to rule out other conditions, such as psoriasis or eczema.
Keratosis Pilaris Risk Factors
There are several risk factors for keratosis pilaris, including:
- Dry skin. People with dry skin are more likely to develop KP.
- Family history. If someone in your family has KP, you are more likely to have it as well.
- Hormonal changes. Hormonal changes, such as those that occur during puberty or pregnancy, can trigger KP.
How keratosis pilaris is treated?
Keratosis pilaris is often a self-limited condition, which means that it will go away on its own without treatment. However, there are some treatments that can help to improve the appearance of KP and to relieve the associated itchiness and irritation.
Here are some common treatments to do:
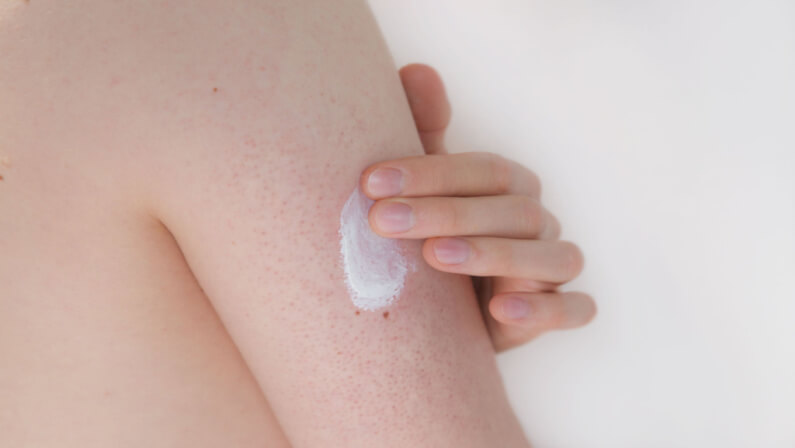
Over-the-counter moisturizing lotions
These can help to hydrate the skin and to reduce the appearance of KP. Look for lotions that contain glycerin, lactic acid, or urea.
Medicated creams
These can help to exfoliate the skin and to reduce the buildup of keratin. Look for creams that contain salicylic acid, lactic acid, or urea.
Prescription medications
If over-the-counter treatments don’t work, your doctor may prescribe a medicated cream or ointment. These are stronger than over-the-counter products and they can be more effective in treating KP.
Laser therapy
In some cases, laser therapy may be recommended. This can help to improve the appearance of KP by reducing the redness and inflammation.
Exfoliating Scrubs
These can help to remove dead skin cells and to reduce the buildup of keratin. Look for scrubs that contain beads or other exfoliating agents.
Gentle skincare
It is important to be gentle when cleansing and exfoliating your skin. Use warm water and a non-abrasive cleanser. Avoid scrubbing the skin too hard.
Moisturize regularly
Dry skin can worsen KP, so it is important to moisturize regularly. Apply a moisturizer after you shower or bathe while your skin is still damp. This will help to lock in moisture.
Keratosis Pilaris Home Remedies
If purchasing over-the-counter treatments or prescription medications isn’t an option for you, there are some home remedies that you can try.
Here are some common home remedies for KP:
- Apply coconut oil. This can help to moisturize the skin and to reduce the appearance of KP.
- Apply apple cider vinegar. This can help to exfoliate the skin and to reduce the redness and inflammation associated with KP.
- Apply a baking soda paste. This can help to exfoliate the skin and to reduce the appearance of KP.
- Use water. Water is a natural moisturizer and it can help to hydrate the skin.
Keratosis Pilaris Prevention
Unfortunately, there is no sure way to prevent KP.
However, there are some things that you can do to reduce your risk of developing the condition:
- Keep your skin hydrated. Dry skin is a risk factor for KP, so it is important to keep your skin hydrated. Drink plenty of water and apply a moisturizer regularly.
- Avoid scrubbing the skin too hard. Scrubbing the skin too hard can irritate it and make KP worse. Be gentle when you are cleansing and exfoliating your skin.
- Use non-abrasive cleansers. Harsh cleansers can irritate the skin and make KP worse. Look for gentle, non-abrasive cleansers.
- Avoid picking at your skin. Picking at your skin can irritate it and make KP worse. If you have the urge to pick at your skin, try to keep your hands busy with something else.
What is the difference between keratosis pilaris and acne
KP is not acne. Acne is a condition that is characterized by the presence of pimples, blackheads, or whiteheads. KP is a condition that is characterized by the presence of small, hard bumps on the skin.
What is the difference between keratosis pilaris and eczema?
KP is not eczema. Eczema is a condition that is characterized by the presence of red, itchy, and inflamed skin. KP is a condition that is characterized by the presence of small, hard bumps on the skin.
What are the long-term effects of keratosis pilaris?
KP is a benign condition that does not have any long-term effects. However, the condition can be cosmetically displeasing and it may cause psychological distress.
Have Your Skin Treated Today!
Keratosis pilaris may be a nuisance, but there are treatments available that can help. If you’re concerned about your KP, talk to a dermatologist today. With the right treatment, you can get rid of those pesky bumps for good!
At Team Dermatology, our team of board-certified dermatologists is an expert in the treatment of keratosis pilaris. We offer a variety of treatments that can help to reduce the appearance of KP, including topical therapies, lasers, and light therapy.
Contact us today to schedule an appointment. We’re here to help you achieve clear, beautiful skin!